Diabetic Foot Care & Wound Services
Diabetic Foot Care is essential for those suffering from diabetes.
Expert Diabetic Foot Care in Maryland
Diabetic Foot Care is essential for those suffering from diabetes. More than 16 million Americans have diabetes and of those, between 10 and 15% will develop a diabetic foot ulcer during their lifetime. These ulcers are commonly found along the bottom of the foot and come with complications like swelling, infection, reduced mobility, and sometimes even a need for hospitalization. Nationwide, diabetes is the leading cause of non traumatic foot amputations. But 75% to 85% of foot amputations are preceded by foot ulcers. This means if we can intervene early to limit the damage caused by an ulcer, we may be able to delay amputation or prevent it entirely.
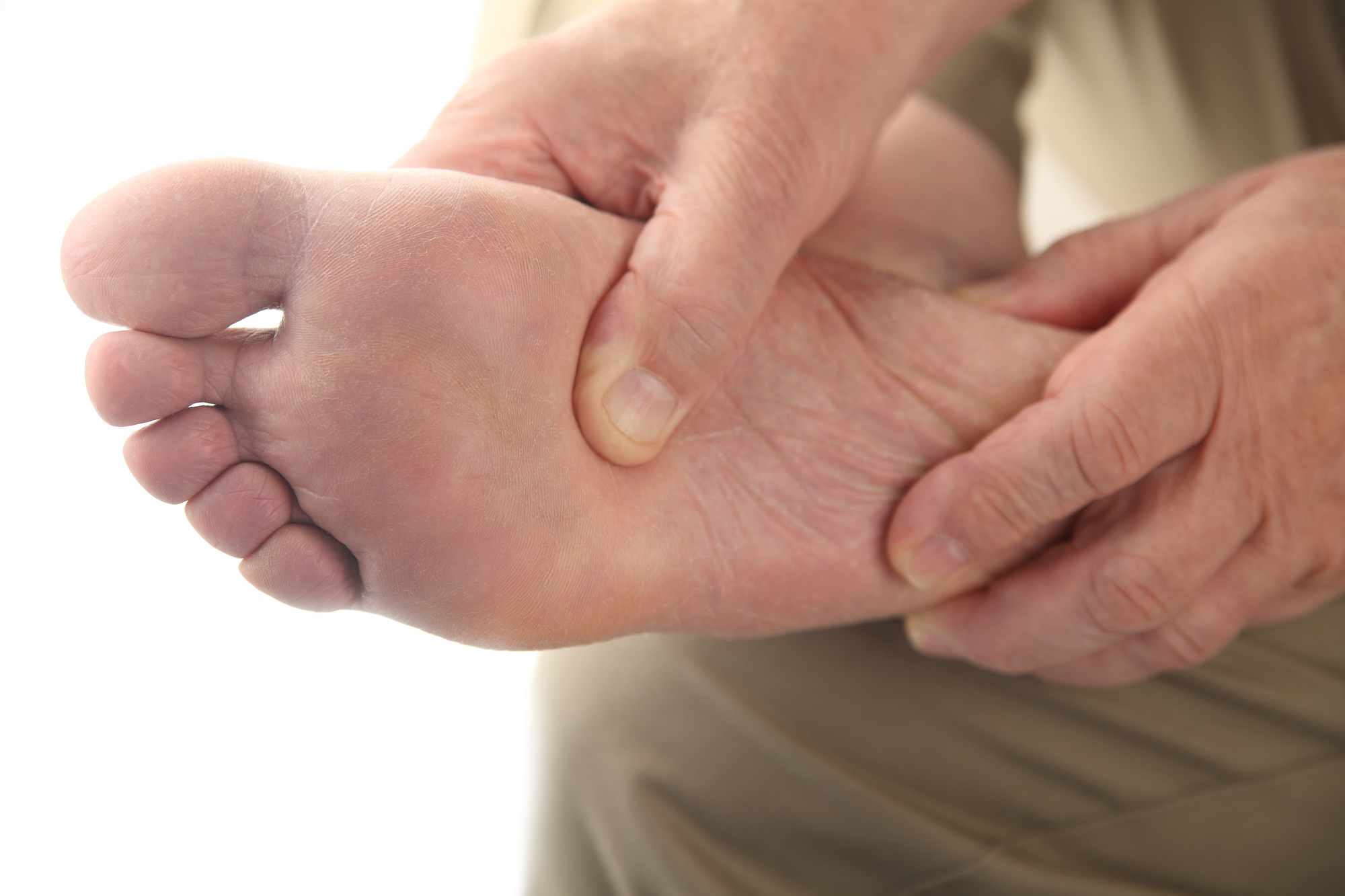
Diabetic Foot Care Can Prevent Foot Ulcers
WHAT CAUSES A DIABETIC FOOT ULCER?
Diabetic foot ulcers are open sores that occur on the foot, primarily on the sole. They are often accompanied by seeping, swelling, and infections and they tend to become much worse without treatment. Over time, it may become quite difficult to walk due to these wounds.
The causes of diabetic foot ulcers are varied and people with chronic ulcers can have a combination of contributing factors. Common factors, beyond having diabetes, include:
Additional contributing factors include being over 45 and being of Native American, African American, or Hispanic origin. These groups have both a higher incidence of diabetes and a higher risk of diabetic foot ulcers.
DIABETIC FOOT CARE BEGINS WITH UNDERSTANDING SYMPTOMS
SYMPTOMS OF A DIABETIC FOOT ULCER
One of the most important things to know about diabetic foot ulcers is that pain is not a primary symptom. The person with the ulcer may not sense much pain due to the advanced stage of their diabetes.
When someone has diabetes for a long period of time, they sometimes develop neuropathy, or numbness due to nerve damage. For this reason, it’s critical to notice these early symptoms of diabetic foot ulcers:


Take these symptoms seriously and see a podiatrist right away. A podiatrist offers simple, painless tests for nerve damage and other issues related to foot wounds. The faster you seek treatment for a diabetic foot wound, the better your prognosis will be.
Your Podiatrist is Your Partner in Diabetic Foot Care
"When do I need to see a podiatrist for diabetic foot issues?"
You may have heard the common saying, “an ounce of prevention is worth a pound of cure”. Professional diabetic foot care can prevent the loss of a limb for diabetics. The truth is that a simple hangnail or pressure sore can turn into a non-healing wound. Instead of waiting until you have a non-healing wound or diabetic foot ulcer, it is best to have regular checkups and preventative care from a podiatrist. Properly trimmed toenails and proper foot care may keep you from requiring more advanced treatments. Doctors of Podiatric Medicine (DPM) are uniquely qualified for diabetic foot care and can spot problems, often before you even know you have one. When you see a podiatrist about a foot care concern related to diabetes, many factors will be considered. Your podiatrist may ask about your family history, examine your feet, and discuss lifestyle concerns like your choice of footwear. A podiatrist helps intervene as early as possible, ideally before a diabetic foot wound reaches an advanced or chronic state. The podiatrist may recommend treatments like:
Family Podiatry is Here for All Your Diabetic Foot Care Needs

Preventing Diabetic Foot Wounds
WHAT CAUSES A DIABETIC FOOT ULCER?
Prevention is truly the best treatment for a diabetic foot wound because it keeps a wound from developing in the first place. Whether a patient has had a foot wound in the past or is simply being proactive, here are some best practices for prevention of diabetic foot wounds:
It is a myth that diabetic foot wounds should be kept dry and aired out. Healing actually occurs faster when patients keep wounds covered with an appropriate bandage and retain the moisture needed for proper healing. Topical treatments may further assist with healing.
However, don’t go too far in caring for the wound and assume more moisture is better. Do not soak a diabetic foot wound unless specifically instructed to do so by your doctor and avoid whirlpools and public pools where there is a risk of spreading infection.
It is essential to learn how to do a daily foot check as part of diabetic foot care. Check your feet thoroughly every day in a methodical way. Take particular care in looking at the sole of your foot and between your toes. Report any of the following to your podiatrist: redness, swelling, bruises, cuts, cracks, blisters, and changes to the shape of your foot
3 Convenient Locations
Reisterstown
Address:
4 Glyndon Drive, Suite 2A
Reisterstown, MD 21136
Towson
Address:
7600 Osler Drive, Suite 105
Towson, MD 21204
Baltimore- Rotunda
Address:
711 W. 40th Street, Suite 351
Baltimore, 21211
Contact the Family Podiatry of Maryland Team
Interested in booking at one of our three convenient locations? Feel free to send us a message so we can reach out to you as soon as possible! We're here to help with all your foot and ankle needs.